Theme: To Transform and connect innovative therapies in Diabetes and Endocrinology
Venue: Panorama Hotel Prague Milevská 7, 140 63 PrahaWorld Endocrinology 2019
- About the World Endocrinology 2019
- Welcome Message
- Who should attend?
- Why to Attend?
- Abstract Eligibility Criteria
- Major Sessions
- Market Analysis
- Past Conference Report
Conference series is hosting the 15th World Congress on Endocrinology and Diabetes (World Endocrinology 2019) at Prague, Czech Republic during September 20-21, 2019.World Endocrinology 2019 Conference is based on the theme of To "Transform and connect innovative therapies in Diabetes and Endocrinology."
World Endocrinology 2019 welcomes all the Endocrinologists, Diabetologists, and other medical & clinical experts working the arena of Endocrinology, Metabolic Syndrome and related field to this upcoming World Endocrinology 2019 Prague, Czech Republic.
Welcome Message from Prof. Francesco Lippi
Dear Friends, Endocrinologists, Diabetologist and other Medical and Clinical experts, Students and Nurses, it’s a great pleasure and privilege to invite you to join the 15th World Congress of Endocrinology & Diabetes in September 2019 in Prague.
Our meeting can be considered the major event in developing, upgrading and teaching the Endocrinology, Diabetes and Metabolic Syndromes. Our Discipline strongly stimulated by the possibilities offered by cellular endocrinology and by the progress in clinical biochemistry and experimental pharmacology, needs this important moment, which can be considered our World Congress. In the same way, the achievements of randomized clinical trials, epidemiological surveys and large meta-analysis will allow us to better understand the possibilities, limits, risks and advantages of our therapies and diagnostic approaches.
The program, developed by the Executive Board, will receive input from Scientific Societies, mostly members of the Endocrine Society that normally cooperates with us. Moreover, the Congress remains open to the suggestions of our Members, Working groups and any other Institution that want to increase the scientific and educational level of the Event.
I strongly hope to receive your proposals for the progress of Endocrinology and Diabetes, and have the pleasure to meet you in Prague in September 2019.
World Endocrinology 2019 welcome the Scientists, Doctors, Academician, Researchers, Students, Business Entrepreneurs, etc. related to the broad areas of Diabetes, Endocrinology, Medical and Health care, Diabetes and Endocrinology organizations are most likely to attend World Endocrinology Congress 2019 and utilize the scope of extending their skills, and their work on basic and significant applications. The World Endocrinology Congress 2019 conference will be useful to participants from both the Industry and Academia working in all the domains of Health care sectors, all other target audience includes:
- Researchers
- Scientists
- Health care experts
- Diabetologists
- Endocrinologists
- Cardiologists
- Nephrologists
- Nutritionists/Dieticians
- Diabetes Health Professionals
- Physicians
- Nurse practitioners
- Health care analysts
- Doctors
- Academic researchers
- Professors
- Students
- Research Institutes
- Business delegates
- Young Researchers
- Advertising and Promotion Agency Executives
- Professionals in media sector
- Medical colleges
- Diabetes Societies & Associations
- Obesity Societies & Associations
- Heart Societies & Associations
- Medical & Pharmaceutical Companies
- Medical devices & companies
- Others
World Endocrinology 2019 conference brings together experts, leading researchers, scholars, scientists, professors from fields of Health care, Endocrinologists, Diabetologists, Nutrition, Physicians, Nurse practitioners and other related areas to interact and exchange ideas about the state of the art technologies related to Endocrinology and Diabetes. The conference will also provide an insightful understanding to the issues arising out of the Endocrinology and Diabetes and the future concern and remedies from that. World Endocrinology 2019 provides an opportunity to interact with eminent Scientists, researchers, Business Leaders, experts from all over the world. The little effort put by the World Endocrinology 2019 will help in taking a giant step in the field of Health care.
Highlights of World Endocrinology 2019 Conference:
- Meet the Health care experts, Endocrinologists, Diabetologists and Nutritionists from 25+ countries around the globe
- Meet your peers and evaluate your research in front of experts
- World-class platform to Exhibit your products and services
- More than 25 presentations from Industry and Academia leader
- One- to-one interaction, B2B, and B2A etc.
- Well organized Scientific Program with 5+ hours of Networking sessions
- Interactive panel discussions and Q&A sessions
- Best Poster Awards, Young Research Forums
AUTHOR ELIGIBILITY:
- Individuals may submit up to two regular abstracts as the first author.
- Individuals may submit an unlimited number of Trials in Progress abstracts.
- Individuals may serve as a co-author on an unlimited number of abstracts.
ABSTRACT ELIGIBILITY
- All types of Diabetes, Endocrinology, Medicinal, Health research are eligible for submission.
- Abstract should address scientific questions, detail clinical observations, or contain primary scientific data.
- Data from the long-term follow-up of previously presented clinical trials may be submitted only if significant new information can be shown.
- Interim analysis of a prospective randomized clinical trial will be considered if it is performed as planned in the original protocol and is statistically valid.
- Abstracts of clinically-related subjects should be combined into a single abstract.
Note: Submission of multiple abstracts on a single study may result in the rejection of one or more abstracts.
Submission Requirements
Provide your full name, academic degree(s), institution, address, and email address and recent photograph. You will receive all future correspondence from us regarding the status of your abstract.
The selected abstracts will be published in Conference Proceedings.Important Dates:
Early Bird Discount Registration Offer: On/Before July 27, 2019
Early Bird Abstract Submission Date: August 24, 2019
Abstract Submission Deadline: September 19, 2019
Speaker Presentations Sessions and Time limits:
Keynote Speech 40-45 Minutes,
Workshop/Symposium 60 Minutes
Plenary Speech 20-25 Minutes,
Poster Presentation 10-15 Minutes
- Endocrinology and Diabetes
- Endocrinology Glands and Hormones
- Diabetes: Types and its Complications
- Pathophysiology: Endocrinology and Diabetes
- EDCs (Endocrine Disrupting Chemicals)
- Endocrine and Diabetes Disorders
- Endocrine and Diabetes Biomarkers
- Diabetes Nephropathy
- Diabetes Retinopathy
- Pediatric endocrinology
- Clinical Gynecologic Endocrinology and Infertility
- Thyroid gland Disorders
- Diabetic & Endocrine Diagnostic Tools and Tests
- Endocrinology: Male & Female Reproductive Health
- Obesity and Metabolic Disorders
- Advance Treatment and Prevention of Diabetes
Tract 01: Endocrinology and Diabetes
Endocrinology is the study of the medical aspects of hormones, including diseases and conditions associated with hormonal imbalance. Endocrinology is the branch of medicine concerned with the structure, function, and disorders of the endocrine glands. Humans have over 50 different hormones. They can exist in very small amounts and still have a significant impact on bodily function and development. The endocrine system consists of several glands, all in different parts of the body that secrete hormones directly into the blood rather than into a duct system. Hormones have many functions and modes of action.
Diabetes is a disease that affects the body’s ability to produce or use insulin. Diabetes is a number of diseases that involve problems with the hormone insulin. Normally, the pancreas releases insulin to help the body store and use the sugar and fat from the food that eat. Diabetes occurs when the pancreas does not produce any insulin, when the pancreas produces very little insulin and when the body does not respond appropriately to insulin, a condition called insulin resistance.
Tract 02: Endocrinology Glands and Hormones
Endocrine Glands
- Hypothalamus: The hypothalamus is located in the brain and links the nervous and endocrine systems to each other.
- Pineal Gland: The pineal gland is a small, pine-cone shaped endocrine gland in the brain. It produces melatonin.
- Pituitary gland: It is located at the base of the brain and is closely connected to the hypothalamus.
- Thyroid: The butter-fly shaped thyroid gland is one of the largest endocrine glands. The thyroid gland is in the front of the neck, just below the thyroid cartilage.
- Parathyroid Gland: The parathyroid gland controls calcium levels in the blood. The parathyroid is a small of glands around by the thyroid gland.
- Thymus: The thymus is a specialized organ of the immune system. The thymus “educates” T-lymphocytes (T cells), which are critical cells of the adaptive immune system.
- Adrenal Glands: The small, triangular adrenal glands located in the kidneys. Each is divided into two distinct anatomic and functional organs that is adrenal cortex and adrenal Medulla.
- Pancreas: The pancreas is a gland organ in the digestive system and endocrine system. It is both an endocrine gland producing several important hormones, including insulin, glucagon, somatostatin, and pancreatic polypeptide and a digestive organ secreting pancreatic juice containing digestive enzymes that help with the absorption of nutrients and digestion in the small intestine.
- Ovaries: The ovary is an ovum-producing reproductive organ, often found in pairs in the female reproductive system.
- Testes: The testicle is the male gonad. The primary functions of the testes are to produce inhibin, sperm and androgens, primarily testosterone.
Endocrine Hormones
- Luteinizing Hormone: This is a pituitary hormone that helps regulate the function of the reproductive organs. It stimulates ovulation to release the egg in the woman’s ovaries.
- Prolactin: This is a pituitary hormone that stimulates the production of milk in the breast. It is one of several hormones that stimulate milk production or lactation.
- Oxytocin: Oxytocin is a pituitary hormone that stimulates muscle contractions in the uterus during childbirth. These contractions cause the release of more oxytocin.
- Glucagon: The hormone glucagon increases the level of sugar in the blood. It plays a vital part in maintaining the correct blood sugar level.
- Reproductive Hormones: Reproductive hormones control the reproductive development of boys and girls.
- Female Reproductive Hormone: Estrogen is the female hormone made mainly in the ovaries. It not only makes the girl reproductive organs develop, and controls her monthly menstrual cycle. Progesterone is the female hormone that prepares the girls uterus for pregnancy every month.
- Male Reproductive Hormone: The male reproductive system consists of the penis, scrotum, and the 2 testes. A male reproductive system creates sperm cells that combined with a female egg to create a new human life. The testes and scrotum hang outside the body where it is cooler because it improves sperm production.
- Epinephrine: Epinephrine is a hormone that works without nervous system to prepare our body to cope with danger or stress. If you’re suddenly scared, your heart pounds, your breathing becomes steep and rapid.
- Insulin: Insulin is a hormone that reduces the level of sugar in our blood. Insulin is a protein made by the pancreas. It is released when the blood sugar level rises and reduces the sugar in 2 ways. First it makes insulin take up the glucose.
Tract 03: Diabetes: Types and its Complications
Types of Diabetes
- Type 1 diabetes: It is usually caused by an auto-immune reaction where the body’s defense system attacks the cells that produce insulin. The reason this occurs is not fully understood. People with type 1 diabetes produce very little or no insulin. The disease may affect people of any age, but usually develops in children or young adults. People with this form of diabetes need injections of insulin every day in order to control the levels of glucose in their blood. If people with type 1 diabetes do not have access to insulin, they will die.
- Type 2 diabetes: It is used to be called non-insulin dependent diabetes or adult-onset diabetes, and accounts for at least 90% of all cases of diabetes. It is characterized by insulin resistance and relative insulin deficiency, either or both of which may be present at the time diabetes is diagnosed. The diagnosis of type 2 diabetes can occur at any age. People with type 2 diabetes can often initially manage their condition through exercise and diet. However, over time most people will require oral drugs and or insulin.
- Gestational diabetes (GDM): It is a form of diabetes consisting of high blood glucose levels during pregnancy. It develops in one in 25 pregnancies worldwide and is associated with complications to both mother and baby. Gestational diabetes usually disappears after pregnancy but women with Gestational diabetes and their children are at an increased risk of developing type 2 diabetes later in life.
Diabetes complication
- Cardiovascular disease: It affects the heart and blood vessels and may cause fatal complications such as coronary artery disease and stroke. Cardiovascular disease is the most common cause of death in people with diabetes. High blood pressure, high cholesterol, high blood glucose and other risk factors contribute to increasing the risk of cardiovascular complications.
- Kidney disease: It is also known is diabetic nephropathy. It caused by damage to small blood vessels in the kidneys leading to the kidneys becoming less efficient or to fail altogether. Kidney disease is much more common in people with diabetes than in those without diabetes. Maintaining near normal levels of blood glucose and blood pressure can greatly reduce the risk of kidney disease.
- Nerve disease: It is also known as diabetic neuropathy. It causes damage to the nerves throughout the body when blood glucose and blood pressure are too high. This can lead to problems with digestion, erectile dysfunction, and many other functions. Among the most commonly affected areas are the extremities, in particular the feet. Nerve damage in these areas is called peripheral neuropathy, and can lead to pain, tingling, and loss of feeling
- Eye disease: It is also known as diabetic retinopathy. In most people with diabetes will develop some form of eye disease causing reduced vision or blindness. Consistently high levels of blood glucose, together with high blood pressure and high cholesterol, are the main causes of retinopathy. It can be managed through regular eye checks and keeping glucose and lipid levels at or close to normal.
- Pregnancy complications: Women with any type of diabetes during pregnancy risk a number of complications if they do not carefully monitor and manage their condition. To prevent possible organ damage to the fetus, women with type 1 diabetes or type 2 diabetes should achieve target glucose levels before conception.
- Oral complications: People with diabetes have an increased risk of inflammation of the gums if blood glucose is not properly managed. Periodontitis is a major cause of tooth loss and is associated with an increased risk of cardiovascular disease.
Tract 04: Pathophysiology: Endocrinology and Diabetes
Endocrine disorders can be classified according to the intensity of hormonal activity and according to the origin of endocrine disorder. From the intensity of hormonal activity of endocrine gland we can distinguish hyper function of endocrine gland, which is characterized by increased secretion of its hormone as well as by increased concentration of this hormone in circulating blood. Hypo function of endocrine gland, which is characterized by decreased secretion of its hormone as well as by decreased concentration of this hormone in circulating blood.
If endocrine gland produces several kinds of hormones the symptoms resulting from hyper production or hypo production of more kinds of hormones may develop, respectively, at the same time the symptoms of hyper function resulting from overproduction of one kind of hormones and the symptoms of hypo function due to a deficiency of other kind of hormones can develop. Eufunction of endocrine gland, which is in the time of medical examination characterized by normal secretion of its hormone as well as by normal concentration of this hormone in circulating blood.
Endocrine disease results when a gland produces too much or too little of an endocrine hormone called as hormone imbalance. Diabetic Ketoacidosis is caused in type 1 diabetes where there is complete lack of insulin and reliance on fatty acids for energy. This uncontrolled lipid breakdown leads to formation of ketones and causes acidosis and ketonemia. This is a medical emergency.
Non-Kenotic Hyperosmolarity – this is caused due to extreme rise of blood sugar. This is seen in type 2 diabetics. There is just enough insulin to suppress ketone synthesis. The high blood sugar leads to excessive concentration or osmolality of blood which in turn leads to dieresis and collapse of the blood vessels and cardiovascular shock. This is a medical emergency.
Tract 05: Endocrine and Diabetes Disorders
- Endocrine Disorders causes when a gland produces too much or too little of an endocrine hormone, called a hormone imbalance and due to development of lesions in the endocrine system, which may or may not affect hormone levels.
- Adrenal insufficiency: The adrenal gland releases too little of the hormone cortisol and sometimes, aldosterone. Symptoms include fatigue, stomach upset, dehydration, and skin changes.
- Cushing's disease. Overproduction of a pituitary gland hormone leads to an overactive adrenal gland. A similar condition called Cushing's syndrome may occur in people, particularly children, who take high doses of corticosteroid medications.
- cromegaly and other growth hormone problems. If the pituitary gland produces too much growth hormone, a child's bones and body parts may grow abnormally fast. If growth hormone levels are too low, a child can stop growing in height.
- Hyperthyroidism. The thyroid gland produces too much thyroid hormone, leading to weight loss, fast heart rate, sweating, and nervousness. The most common cause for an overactive thyroid is an autoimmune disorder called Grave's disease.
- Hypothyroidism. The thyroid gland does not produce enough thyroid hormone, leading to fatigue, constipation, dry skin, and depression. The underactive gland can cause slowed development in children
- Hypopituitarism. The pituitary gland releases little or no hormones. It may be caused by a number of different diseases. Women with this condition may stop getting their periods.
- Multiple endocrine neoplasia: These rare, genetic conditions are passed down through families. They cause tumors of the parathyroid, adrenal, and thyroid glands, leading to overproduction of hormones.
- Polycystic ovary syndrome (PCOS). Overproductions of androgens interfere with the development of eggs and their release from the female ovaries. PCOS is a leading cause of infertility.
- Precocious puberty. Abnormally early puberty that occurs when glands tell the body to release sex hormones too soon in life.
Tract 06: Endocrine Disrupting Chemicals
An Endocrine Disrupting Chemical (EDC) or Endocrine Disruptor (ED) is any chemical that can interfere with normal hormone functions in humans and/or Endocrine Disrupting Chemical animals. The human endocrine system is a collection of glands which secrete different types of hormones that regulate the body’s growth and metabolism, sexual development, and behavior. Naturally occurring hormones are usually active at very low doses. A healthy endocrine system is essential to the normal functioning of the human body.
Some EDCs are present in our natural environment including phytoestrogens however, most EDCs are synthetic compounds. Over a 1400 compounds are known or suspected to be EDCs. Only a small fraction of these has been investigated in tests capable of identifying endocrine effects in intact organisms. EDCs are present in a wide variety of products including plastics, pesticides, cosmetics, fragrances, food, kitchen cleaners, adhesives, paints, clothing, medical equipment, and toys.
In 2015 the Endocrine Society released a statement on endocrine-disrupting chemicals (EDCs) specifically listing obesity, diabetes, female reproduction, male reproduction, hormone-sensitive cancers in females, prostate cancer in males, thyroid, and neurodevelopment and neuroendocrine systems as being affected biological aspects of being exposed to EDCs. The critical period of development for most organisms is between the transitions from a fertilized egg into a fully formed infant. As the cells begin to grow and differentiate, there are critical balances of hormones and protein changes that must occur. Therefore, a dose of disrupting chemicals may do substantial damage to a developing fetus. The same dose may not significantly affect adult mothers.
Tract 07: Endocrine and Diabetes Biomarkers
A biomarker is defined as any substance, structure, or process that can be measured in the body or its products and influence or predict the incidence of outcome or disease. For the purpose of predicting type 1 diabetes, a biomarker should be present in a subset of the population, and this subset should have a bias in the proportion of people in whom type 1 diabetes develops. A biomarker should also present a quantifiable risk for the development of type 1 diabetes within a defined period or diagnose a “stage” in the progression to clinical or symptomatic type 1 diabetes. As described in this article, most of the biomarkers used for the prediction of type 1 diabetes are islet-specific supporting the concept that, before overt hyperglycemia, type 1 diabetes is predominantly a targeted disease rather than a systemic disease.
Atomic Biomarkers can be separated as "a trademark that is precisely measured and gaged as a pointer of typical natural methods, pathogenic methodology, or pharmacologic reactions to a pharmaceutical intercession.
Biomarkers have fundamental influence in driving clinical trials and treating patients. Progresses in sub-atomic diagnostics help medicinal experts make proficient, experimentally legitimate choices. All the more efficient disclosure and use of biomarkers in the development of ant diabetes medications will rely on upon quickening our comprehension of the pathogenesis of diabetes and particularly its macro vascular entanglements. Procedural upgrades from different fields, particularly tumor, are starting to demonstrate the way towards better models of diabetes pathogenesis and atomic biomarker revelation.
- Prognostic marker
- Diabetic nephropathy marker
- Molecular marker for metabolic syndrome
- Molecular Marker-Hypoglycemic response
- Inflammatory markers: Type 2 diabetes
- Pharmacotherapy in treatment of diabetes
Tract 08: Diabetic Nephropath
People with diabetes, the small blood vessels in the body are injured. When the blood vessels in the kidneys are injured, kidneys cannot clean the blood properly. The body will retain more water and salt than it should, which can result in weight gain and ankle swelling. Results may have protein in the urine. Also, waste materials will build up in the blood. Diabetes also may cause damage to nerves in the body. This can cause difficulty in emptying the bladder. The pressure resulting from the full bladder can back up and injure the kidneys. Also, if urine remains in the bladder for a long time, it can develop an infection from the rapid growth of bacteria in urine that has a high sugar level.
The earliest sign of diabetic kidney disease is an increased excretion of albumin in the urine. Weight gain and ankle swelling may occur. The blood pressure may get too high. As a person with diabetes, you should have your blood, urine and blood pressure checked at least once a year. This will lead to better control of disease and early treatment of high blood pressure and kidney disease. Maintaining control of the diabetes can lower the risk of developing severe kidney disease.
Signs of Kidney Disease in Patients with Diabetes
- Albumin/protein in the urine
- High blood pressure
- Ankle and leg swelling, leg cramps
- Going to the bathroom more often at night
- High levels of BUN and creatinine in blood
- Less need for insulin or antidiabetic medications
- Morning sickness, nausea and vomiting
- Weakness, paleness and anemia
- Itching
Tract 09: Diabetic retinopathy
Chronically high blood sugar from diabetes is associated with damage to the tiny blood vessels in the retina, leading to diabetic retinopathy. The retina detects light and converts it to signals sent through the optic nerve to the brain. Diabetic retinopathy can cause blood vessels in the retina to leak fluid or hemorrhage, distorting vision. In its most advanced stage, new abnormal blood vessels proliferate on the surface of the retina, which can lead to scarring and cell loss in the retina.
People with all types of diabetes are at risk for diabetic retinopathy. Risk increases the longer a person has diabetes. Between 40 and 45 percent of Americans diagnosed with diabetes have some stage of diabetic retinopathy, although only about half are aware of it? Women who develop or have diabetes during pregnancy may have rapid onset or worsening of diabetic retinopathy
- Symptoms and Detection
- Causes and risk factors
- Diagnosis and Tests
- Prevention and Treatment
- Current Research
Tract 10: Pediatric endocrinolog
Pediatric endocrinology deals with the disorders of the endocrine glands, such as variations of physical growth and sexual development in childhood, diabetes and many more. The most common disease of the specialty is type 1 diabetes, which usually accounts for at least 50% of a typical clinical practice. The next most common problem is growth disorders, especially those amenable to growth hormone treatment.
Pediatric endocrinologists are usually the primary physicians involved in the medical care of infants and children with intersex disorders. The specialty also deals with hypoglycemia and other forms of hyperglycemia in childhood, variations of puberty, as well other adrenal, thyroid, and pituitary problems. Many pediatric endocrinologists have interests and expertise in bone metabolism, lipid metabolism, adolescent gynecology, or inborn errors of metabolism.
Tract 11: Clinical Gynecologic Endocrinology and Infertility
- Obstetrics and Gynecology: Obstetrics deals with the care of the pregnant women, the unborn baby, labor and delivery and the immediate period following childbirth. The obstetrician ensures that mother and child get the best prenatal care to ensure labor and delivery is accomplished without complications and that should intervention be needed, it is done quickly and safely. Gynecology deals with any ailment concerning the reproductive organs; uterus, fallopian tubes, cervix, ovaries and vagina. A gynecologist may also treat related problems in the bowel, bladder and urinary system since these are closely related to female reproductive organs.
- Clinical Endocrinology: Normal and Abnormal Sexual Development, Abnormal Puberty and Growth Problems, Amenorrhea, Anovulation and the Polycystic Ovary, Hirsutism, Menstrual Disorders, Dysfunctional Uterine Bleeding, Menopause and the Perimenopausal Transition, Postmenopausal Hormone Therapy
- Infertility: Female Infertility, Recurrent Early Pregnancy Losses, Endometriosis, Male Infertility, Induction of Ovulation, Assisted Reproduction, Ectopic Pregnancy
- Contraception: Reproduction and the Thyroid, Family Planning, Sterilization, and Abortion, Oral Contraception, Long-Acting Methods of Contraception, the Intrauterine Device (IUD), Barrier Methods of Contraception
Tract 12: Thyroid glands Disorders
Goiters: A goiter is a bulge in the neck. A toxic goiter is associated with hyperthyroidism, and a non-toxic goiter, also known as a simple or endemic goiter, is caused by iodine deficiency.
Hyperthyroidism: Hyperthyroidism is caused by too much thyroid hormone. People with hyperthyroidism are often sensitive to heat, hyperactive, and eat excessively. Goiter is sometimes a side effect of hyperthyroidism. This is due to an over-stimulated thyroid and inflamed tissues, respectively.
Hypothyroidism: Hypothyroidism is a common condition characterized by too little thyroid hormone. In infants, the condition is known as cretinism. Cretinism has very serious side effects, including abnormal bone formation and mental retardation. If you have hypothyroidism as an adult, you may experience sensitivity to cold, little appetite, and overall sluggishness. Hypothyroidism often goes unnoticed, sometimes for years, before being diagnosed.
Solitary thyroid nodules: Solitary nodules, or lumps, in the thyroid are actually quite commonin fact, it’s estimated that more than half the population will have a nodule in their thyroid. The great majority of nodules are benign. Usually, a fine needle aspiration biopsy (FNA) will determine if the nodule is cancerous.
Thyroid cancer: Thyroid cancer is fairly common, though long-term survival rates are excellent. Occasionally, symptoms such as hoarseness, neck pain, and enlarged lymph nodes occur in people with thyroid cancer. Thyroid cancer can affect anyone at any age, though women and people over thirty are most likely to develop the condition.
Thyroiditis: Thyroiditis is an inflammation of the thyroid that may be associated with abnormal thyroid function. Inflammation can cause the thyroid’s cells to die, making the thyroid unable to produce enough hormones to maintain the body's normal metabolism. There are five types of thyroiditis, and the treatment is specific to each.
Tract 13: Diabetic & Endocrine Diagnostic Tools and Tests
- Adrenal Venous Sampling for Aldosterone, Androgen Levels, Angiography, Arginine Stimulation Test, Arterial Stimulation with Venous Sampling, Autonomic Function Tests
- Basal Acid Output (BAO), Bilateral Simultaneous Inferior Petrosal Sinus Sampling (IPSS) with CRF, Bone Marrow Aspirate
- C-peptide Suppression Test, Calcium Infusion Test for Medullary Cancer of the Thyroid, Captopril Test, Clomiphene Test, Clonidine Suppression Test, Combined Pituitary Function Tests (CPT), Cortisol Day Curve, CRH Test
- Glycated hemoglobin (A1C) test, Exercise Test, Fasting Test, Fine Needle Aspiration of a Thyroid Nodule (FNA), Finger Size Assessment, Gastric Acid Secretion, Glucagon Test, Glucose Tolerance Test, Gonadotrophin Releasing Hormone GnRH/LHRH Test
- High Dose Dexamethasone Suppression Test, Hydrocortisone Day Curve (HCDC), Hydroxycorticosterone (18-OHB) and - cortisol (18-OHF) Tests, Hyperaldosteronism Investigations, Hyperparathyroidism Investigations
- Insulin Tolerance Test, Insulin: Glucagon Ratio, Intravenous Secretin Test, Investigating Systemic Mastocytosis, Ischemic Lactate Test
- Long Synacthen Test, Low Dose Dexamethasone Suppression Test, Measuring Skin-fold Thickness, MIBG Scan
- Octreoscan, Operative Management of Pituitary Tumours, Oral Glucose Tolerance Test for Acromegaly, Overnight Dexamethasone Suppression Test
- Pentagastrin Test for Medullary Cancer of the Thyroid, Pentolinium Suppression Test, Percutaneous Trans-hepatic Portal Venous Sampling, Peripheral Venous Sampling for Ectopic Sources of ACTH, Petrosal Sinus Sampling, Post-Operative Investigation of Thyroid Carcinoma, Posture Studies, Pro-insulin and C-peptide, Prolonged Supervised Fast
- Radioactive Iodine Test, Screening for Ovulation, Selective Arterial Injection for the Localization of Gastrinomas and Insulinomas, Selenium Cholesterol Scanning for Conn's Tumours
- Short Synacthen Test, Somatostatin Receptor Scintigraphy
- Technetium Scan, Therapeutic Trial of ddAVP, Thyrotrophin Releasing Hormone (TRH) Test, Tolbutamide Test, Ultrasound, Visual Field Testing (Goldmann perimetry), Water Deprivation Test
Tract 14: Obesity and Metabolic Disorders
Obesity is mostly preventable through a combination of social changes and personal choices. Changes to diet and exercising are the main treatments. Diet quality can be improved by reducing the consumption of energy-dense foods, such as those high in fat or sugars, and by increasing the intake of dietary fiber. Medications can be used, along with a suitable diet, to reduce appetite or decrease fat absorption. If diet, exercise, and medication are not effective, a gastric balloon or surgery may be performed to reduce stomach volume or length of the intestines, leading to feeling full earlier or a reduced ability to absorb nutrients from food.
A metabolic disorder occurs when the metabolism process fails and causes the body to have either too much or too little of the essential substances needed to stay healthy. Metabolic disorders can take many forms i.e. a missing enzyme or vitamin that’s necessary for an important chemical reaction, abnormal chemical reactions that hinder metabolic processes and disease in the liver, pancreas, endocrine glands, or other organs involved in metabolism
Nutritional deficiencies. Metabolic disorders can be present at birth, and many can be identified by routine screening. If a metabolic disorder is not identified early, then it may be diagnosed later in life, when symptoms appear. Specific blood and DNA tests can be done to diagnose genetic metabolic disorders. The gut microbiota, which is a population of microorganisms that live in the human digestive system, also has an important part in metabolism and generally has a positive function for its host. In terms of pathophysiological/mechanism interactions, an abnormal gut microbioma can play a role in metabolic disorder related obesity.
Tract 15: Endocrinology: Male & Female Reproductive Health
Reproductive Endocrinology is a sub-specialty of Obstetrics and Gynecology. Reproductive endocrinologist is a very important part of obstetrics and gynecology in which physician is trained in reproductive medicine explaining about hormonal functioning as it indirectly relate to reproduction. They are trained to evaluate and treat malfunctioning in females and males outside infertility. Reproductive endocrinologists have special training in obstetrics and gynecology before they undergo sub-specialty training in Reproductive endocrinology and infertility.
Female endocrinology
Female endocrinology has to do largely with the reproductive cycle driven by estrogen and other cyclical female hormones. Related issues that the endocrinologist may help evaluate and provide care for include:
- Early or delayed menarche
- Menstrual irregularity
- Heavy, light or absent menses
- Premenstrual syndrome
- Abnormalities that may produce symptoms that cycle with menses, such as ovarian cysts or uterine fibroids
- Perimenopause
- Menopause
- Endocrine-related depression, fatigue or reduced sex drive
- Hormone replacement therapy
Male Endocrinology
The glands testes produce abnormally low amounts of testosterone, may receive testosterone replacement therapy. For some men, lower than normal testosterone produces no apparent effects; for others, effects of this condition may include:
- Reduced sexual function, in terms of desire, erections and fertility
- Insomnia or other sleep problems
- Reduced muscle size and strength, more body fat and lower bone density
- Emotional changes, such as less confidence and motivation, lower mood and difficulty in concentration and memory.
Tract 16: Transgender: Medicine and Research
- Throughout human history, there have been people who were transgender, individuals whose gender identity and expression differ from the sex they appear to be at birth. Some cultures accepted these differences, whereas others violently opposed them. The current world culture is in the midst of a sea change with regard to gender. And although there is still open hostility in some sectors, in many places, there is an increased openness toward people who are gender-nonconforming.
- Transgender people have a gender identity or gender expression that differs from their assigned sex. Transgender people are sometimes called transsexual if they desire medical assistance to transition from one sex to another. Transgender is also an umbrella term: in addition to including people whose gender identity is the opposite of their assigned sex it may include people who are not exclusively masculine or feminine.
- Being transgender is independent of sexual orientation: transgender people may identify as heterosexual, homosexual, bisexual, asexual, or may decline to label their sexual orientation. The term transgender is also distinguished from intersex, a term that describes people born with physical sex characteristics "that do not fit typical binary notions of male or female bodies”. The counterpart of transgender is cisgender, which describes persons whose gender identity or expression matches their assigned sex.
Tract 17: Advance Treatment and Prevention of Diabetes
Check your risk of diabetes: Risk assessment test and learn more about your risk of developing type 2 diabetes. A 12+ score indicate that you are at high risk and may be eligible for the Life! Program - a free Victorian lifestyle modification program that helps you reduce your risk of type 2 diabetes and cardiovascular disease.
Manage your weight. Excess body fat, particularly if stored around the abdomen, can increase the body’s resistance to the hormone insulin. This can lead to type 2 diabetes.
Exercise regularly. Moderate physical activity on most days of the week helps manage weight, reduce blood glucose levels and may also improve blood pressure and cholesterol.
Eat a balanced, healthy diet. Reduce the amount of fat in the diet, especially saturated and trans fats. Eat more fruit, vegetables and high-fiber foods. Cut back on salt.
Limit takeaway and processed foods. ‘Convenience meals’ are usually high in salt, fat and kilojoules. It’s best to cook for yourself using fresh ingredients whenever possible.
Limit your alcohol intake. Too much alcohol can lead to weight gain and may increase your blood pressure and triglyceride levels. Men should have no more than two standard drinks a day and women should have no more than one.
Quit smoking. Smokers are twice as likely to develop diabetes as non-smokers.
Control your blood pressure. Most people can do this with regular exercise, a balanced diet and by keeping a healthy weight. In some cases, it might need medication prescribed by the doctor.
Reduce your risk of cardiovascular disease. Diabetes and cardiovascular disease have many risk factors in common, including obesity and physical inactivity.
Call for proposals are open for oral papers, panel presentations and scientific posters across the list of tracks highlighted in our website and papers on other topics not listed are also welcome if they meet the objectives of the conference. We hope and expect World Endocrinology 2019 theme to inspire a number of research avenues, and look forward to discussing ideas, findings and synergies, in this International Academic Forum.
Growing incidences of endocrine disorders such as hyperthyroidism and adrenal insufficiency is predicted to boost the demand for endocrine testing.The growing diabetic, geriatric and obese population worldwide is expected to promote the market growth. Furthermore, growing healthcare awareness among individuals coupled with increasing government support is expected to increase the diagnosis at an early, thereby contributing to the growth of the endocrine testing market.
Owing to increasing health awareness around the world, there have been advancement in home health care along with easy operating home diagnostic kits which are cost effective and designed with precision. Many new mass spectrometric technologies have been introduced which deliver accurate results in less time and they are highly sensitive. Mass Spectrometry is now coupled with liquid chromatography for more precision. Telehealth services have also been introduced by some commercial laboratories and stand-alone clinics.
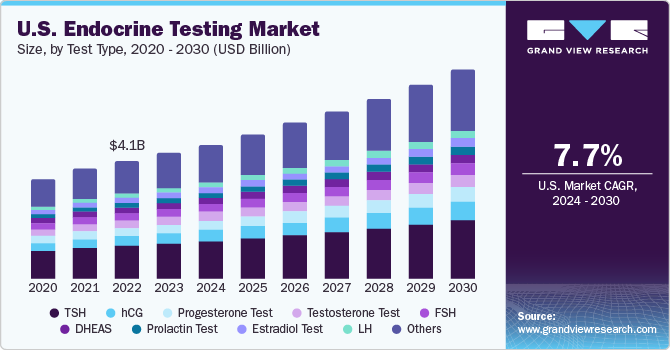
Based on test type, the market is segmented into Estradiol (E2), Human Chorionic Gonadotropin (hCG), Follicle Stimulating (FSH), Dehydroepiandrosterone sulfate (DHEAS), Progesterone, Luteinizing Hormone (LH), testosterone, thyroid prolactin, Thyroid Stimulating Hormone (TSH), cortisol, insulin, and other tests such as gastrin, thymosin, and secretin tests.
Thyroid stimulating hormone (TSH) test accounted for a lucrative share in 2016, This can be attributed to the increasing incidences of TSH-related disorders and the growing awareness regarding correlation between variations in the thyroid hormones levels and cardiovascular disorders.
Insulin test is anticipated to witness the fastest growth over the forecast period. The substantial rise in the diabetic population and the growing awareness about diagnosis are anticipated to contribute towards the demand for insulin test over the forecast period.
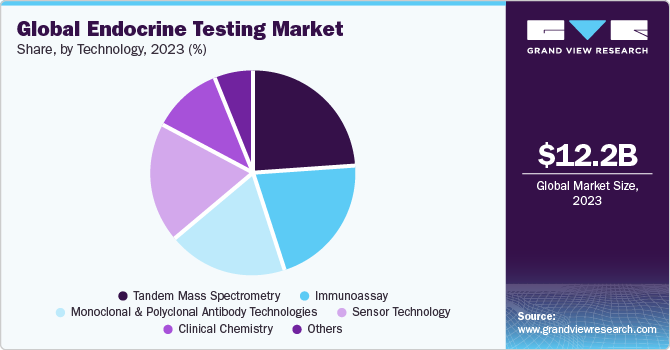
Key technology segments include tandem mass spectrometry, immunoassay, monoclonal & polyclonal antibody technologies, sensors, clinical chemistry technologies, and others such as Liquid Chromatography with Mass Spectrometry (LC-MS).
The tandem mass spectrometry is expected to dominate the market during the forecast period. This can be attributed to growing use of tandem mass spectrometry in combination with liquid chromatography which helps in overcoming the challenges associated with traditional techniques used for endocrine testing.
Sensor Technology is expected to show the fastest growth among all the segments owing to growing use of biosensors in glucose monitoring for diabetes which is used on routine basis by the individuals to monitor their blood sugar level in undiluted blood samples.
The major share in endocrine testing market share is held by companies such as Abbott Laboratories, AB Sciex, Agilent Technologies, Biomedical Technologies, bioMerieux SA, Bio Rad Laboratories, DiaSorin, Hoffmann-La Roche Ltd., LabCorp, and Quest Diagnostics.
The players are actively involved in launching technologically advanced products and initiate collaborative developments to sustain themselves in the competition. For instance, LabCorp offers all-embracing solutions on clinical trials pertaining to diabetes and all other hormonal diseases. In addition, the company also provides liquid chromatography in combination with mass spectrometry to yield specific results even with minimal amounts of the hormonal sample.
The 14th World Congress on Endocrinology & Diabetes (World endocrinology 2018) convoked by Conference Series during November 21-22, 2018 was successfully held at Holiday Inn Paris – Marne La Vallée with a theme Reconnoitering the Challenges Concerning Endocrinology and Diabetes Research” was a great success where eminent keynote speakers from various reputed institutions with their resplendent presence addressed the gathering.
Thanks to all our momentous speakers, conference attendees who contributed towards the successful run of the conference.
World Endocrinology 2018 witnessed an amalgamation of peerless speakers who enlightened the crowd with their knowledge and confabulated on various new-fangled topics related to the fields of Healthcare.
The meeting was carried out through various sessions, in which the discussions were held on the following major scientific tracks:
- Endocrinology: Types and Categories
- Endocrinology Glands and Hormones
- Diabetes: Types and its Complications
- Endocrine and Diabetes Disorders
- Pathophysiology: Endocrinology, Diabetes and Metabolism
- Cardiovascular Endocrinology
- Endocrinology and Diabetes
- History of Endocrinology and Diabetes
- Pediatric endocrinology
- Diabetic & Endocrine Diagnostic Tools and Tests
- Endocrine and Diabetes Biomarkers
- Endocrinologists and Diabetologists
- Clinical Gynecologic Endocrinology and Infertility
- Prostate Cancer and Endocrinology
- Bone and Mineral Metabolism: Transplantation
- Endocrine Ageing and Neoplastic
- Obesity and Metabolic Disorders
- Transgender: Medicine and Research
- Endocrinology: Male & Female Reproductive Health
- Advance Treatment and Prevention
- Clinical Trails and Case Study
- General Endocrine Practice
- Stem Cell Transplantation & Tissue Engineering
- Herbal and Alternative Remedies
- Associations, Societies and Organizations: Endocrinology and Diabetes
- EDCs (Endocrine Disrupting Chemicals)
World Endocrinology 2018 Organizing Committee would like to thank the Moderator of the conference, Denial, who has contributed a lot for the smooth functioning of this event.
World Endocrinology 2018 extends its warm gratitude to all the Keynote Speakers of the event:
- Gerald C Hsu, eclaireMD Foundation, USA
- Joseph F Ndisang, University of Saskatchewan, Canada
- Osokina Irina Vladimirovna, Russian Academy of Science, Russia
Conference Series is privileged to felicitate World Endocrinology 2018 Organizing Committee and Chairs who supported for the success of this event. Conference Series would like to thank every individual participant for the enormous exquisite response. This inspires us to continue organizing events and conferences for further research in the field of Healthcare.
With the valuable feedback received from the participants of World Endocrinology 2018, Conference Series will be glad to announce its next event i.e. 15th World Congress on Endocrinology & Diabetes scheduled for November 19-20, 2019 at Prague, Czech Republic
See you soon at Prague
Conference Highlights
- Endocrinology and Diabetes
- Endocrinology Glands and Hormones
- Diabetes: Types and its Complications
- Diabetic retinopathy
- Pathophysiology: Endocrinology and Diabetes
- EDCs (Endocrine Disrupting Chemicals)
- Endocrine and Diabetes Biomarkers
- Diabetic Nephropathy
- Pediatric endocrinology
- Clinical Gynecologic Endocrinology and Infertility
- Thyroid glands Disorders
- Diabetic & Endocrine Diagnostic Tools and Tests
- Endocrinology: Male & Female Reproductive Health
- Obesity and Metabolic Disorders
- Advance Treatment and Prevention of Diabetes
- Endocrine and Diabetes Disorders
- Transgender: Medicine and Research
To share your views and research, please click here to register for the Conference.
To Collaborate Scientific Professionals around the World
Conference Date September 20-21, 2019 Sponsors & Exhibitors Click here for Sponsorship OpportunitiesSpeaker Opportunity Closed Day 1 Poster Opportunity Closed Click Here to View Useful Links
Special Issues
All accepted abstracts will be published in respective Our International Journals.
- Journal ofEndocrinology & Diabetes Research
- Journal of Endocrinology & Metabolic Syndrome
- Journal of Clinical and Molecular Endocrinology
Abstracts will be provided with Digital Object Identifier by
Theme: To Transform and connect innovative therapies in Diabetes and Endocrinology
Venue: Panorama Hotel Prague Milevská 7, 140 63 PrahaRenowned Speakers
World Endocrinology 2019
Conference Highlights
- Endocrinology and Diabetes
- Endocrinology Glands and Hormones
- Diabetes: Types and its Complications
- Diabetic retinopathy
- Pathophysiology: Endocrinology and Diabetes
- EDCs (Endocrine Disrupting Chemicals)
- Endocrine and Diabetes Biomarkers
- Diabetic Nephropathy
- Pediatric endocrinology
- Clinical Gynecologic Endocrinology and Infertility
- Thyroid glands Disorders
- Diabetic & Endocrine Diagnostic Tools and Tests
- Endocrinology: Male & Female Reproductive Health
- Obesity and Metabolic Disorders
- Advance Treatment and Prevention of Diabetes
- Endocrine and Diabetes Disorders
- Transgender: Medicine and Research
To share your views and research, please click here to register for the Conference.
To Collaborate Scientific Professionals around the World
Conference Date September 20-21, 2019 Sponsors & Exhibitors Click here for Sponsorship OpportunitiesSpeaker Opportunity Closed Day 1 Poster Opportunity Closed Click Here to View Media Partners